Fixing Shawn’s Heart: Shutting the Door on Another Stroke
- UPMC Passavant-McCandless
- Mar 31, 2023
- 6 min read
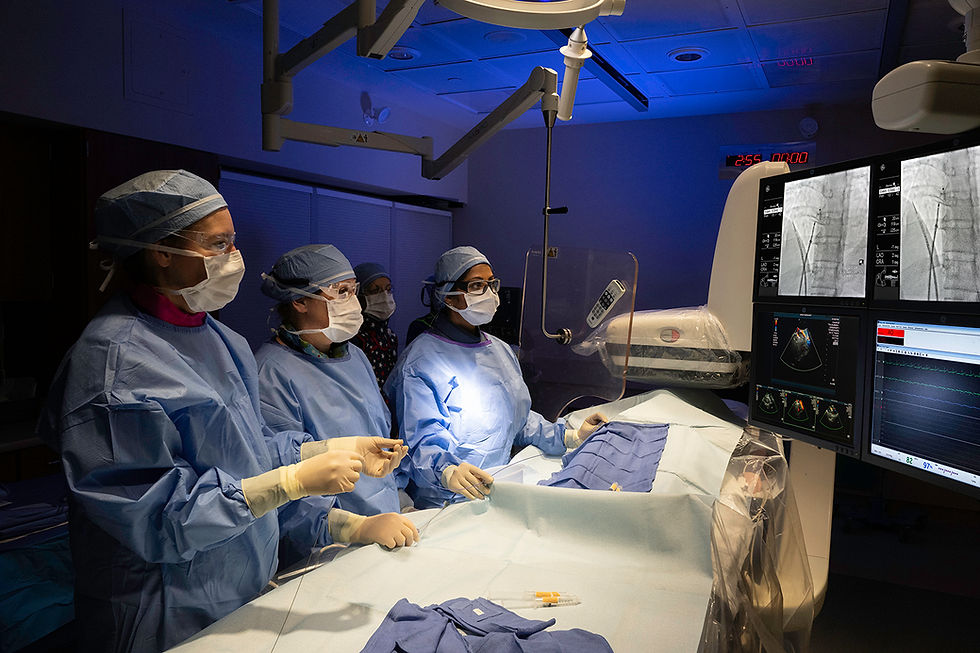
When a stroke led to the discovery of a structural heart defect, Shawn Klik, 45, of New Castle, PA, was referred to cardiologist Amber Makani, MD, at UPMC Passavant. The interventional and structural cardiology specialist used an advanced, minimally invasive procedure to close the hole in his heart — all in under an hour and without the need for open heart surgery.

It was the first day of school in August 2022 when Shawn Klik felt a strange sensation along his left side. A behavioral intervention specialist with Sharon City School District, Shawn was meeting with a social skills group to review expectations for the year.
“One minute I was standing up talking to students, and the next minute I felt a numbness radiating down my left arm and hip, and into the left side of my neck,” says Shawn. “Then I felt nauseous.”
Although the symptoms went away quickly, Shawn couldn’t shake a lingering uneasiness. At home, he explained to his wife what happened, then called a friend who is a nurse. At her urging, he went to the UPMC Jameson Emergency Department where he was immediately put into stroke protocol.
STROKE DIAGNOSIS AND A CAUSE
At the hospital, Shawn was diagnosed with a transient ischemic attack (TIA), also known as a “mini-stroke.” TIAs occur when blood flow to the brain suddenly stops for a short time, causing stroke-like symptoms. Unlike a stroke, a TIA does not kill brain cells. So, there is no lasting damage.

After reviewing his symptoms with doctors, Shawn recalled another episode decades earlier. “It happened in my 20s when I was hanging out with friends. I stood up and felt numbness on one side and ringing in my ears,” he says. “It went away quickly, so I didn’t think much about it. But looking back, it was very similar.”
It is uncommon for people under the age of 55 to experience a stroke, so Shawn’s doctors performed tests to determine the cause. An echocardiogram revealed he had an abnormality — a hole in his heart known as a patent foramen ovale (PFO).
ELIMINATING THE RISK
Although Shawn recovered from the TIA, surgery was recommended to close the PFO — a procedure that can only be performed by a specialist. He was then referred to Dr. Makani.
According to Dr. Makani, one in four adults has a PFO — a hole between the left and right atrium that never closed the way it should after birth. For most people, having a PFO isn’t a problem. But for some, the opening acts as a portal for blood clots to travel from the body, through the heart and to the brain, causing a stroke.

“The younger the patient, the more concerned we are that the stroke or TIA was caused by a PFO,” says Dr. Makani. “Shawn already had experienced two TIAs. We wanted to prevent it from happening again.”
Shawn, the father of two young sons, agreed. “It was a no brainer,” he says. “I have a family. I figured, if I can keep myself healthy and prevent a stroke, then let’s do it.”
FINDING CLOSURE
On Nov. 15, Dr. Makani performed the PFO closure during a minimally invasive, catheter-based procedure at UPMC Passavant–McCandless. After making a small incision in the groin area, she advanced an ultrasound imaging device through a vein up to his heart. “It gives us a very good view of the heart,” she says.
She then inserted the PFO closure device and guided it up to the heart where it was deployed — two discs each about the size of a half-dollar straddling each side of the hole. “This stops the abnormal blood flow between the two chambers of the heart,” explains Dr. Makani. “Once the catheter is removed, the procedure is complete.”
The procedure took less than one hour. After two hours in recovery for observation and an echocardiogram that confirmed the device was still positioned properly, Shawn was able to go home.
“The whole experience was great. Dr. Makani and her team explained everything and answered all my questions. It really put me at ease,” says Shawn.
“All I felt was a little soreness in the groin area after the surgery. But I had peace of mind knowing that procedure eliminated the possibility of future issues.”
Expanded Heart Care at UPMC Passavant
The UPMC Heart and Vascular Institute at UPMC Passavant now offers two state-of-the-art, minimally invasive surgical procedures to repair holes in the heart: atrial septal defect (ASD) and patent foramen ovale (PFO). Both types of holes can be repaired with a closure device inserted via a catheter threaded from the groin through the veins to the heart.
UPMC cardiologists prefer to use minimally invasive approaches when possible because patients generally have a reduced risk of infection, spend less time in the hospital, and have an overall faster recovery.
WHAT IS AN ASD?
An ASD is a congenital heart condition that occurs when the septal tissue doesn’t form correctly, allowing blood to flow abnormally between the left and right atria. Over time, ASDs can progress to cause damage to the heart and lungs and may need to be treated.
WHAT IS A PFO?
A PFO is a heart defect that occurs when the foramen ovale fails to close after birth. This can result in blood traveling directly from the right atrium to the left. If the blood contains a clot, it can cause a stroke.
These procedures are the latest example of the expanded heart and vascular care and advanced technology now available at UPMC Passavant — making it convenient for patients living in Pittsburgh’s northern suburbs and beyond.
Detecting Heart Disease Before It Strikes
At UPMC Passavant, cardiovascular specialists are focusing efforts on early detection and prevention of heart disease — the nation’s number one killer.

John Hornick, MD, is on a mission to stop heart disease in its tracks before it strikes and symptoms develop.
“The earlier we can identify those at risk, the more we can do to prevent heart attacks and other cardiac events in the future,” says Dr. Hornick, a cardiologist and vascular medicine specialist at UPMC Passavant.
STOPPING A KILLER
Cardiovascular disease, which includes heart attack and stroke, is the leading cause of death for both men and women in the United States.
For some, there are warning signs like chest pain and trouble breathing, especially with activity. But many people don’t realize that they have coronary artery disease — a buildup of plaque in the arteries supplying blood to the heart — so they don’t make lifestyle changes or take the medicines they need to prevent a heart attack, stroke, or death. Others don’t realize their family history of heart disease makes them more likely to develop the condition, too.
“Even without obvious symptoms, people can be at risk,” says Dr. Hornick. “That is why prevention is so important.”
PREVENTING HEART DISEASE
According to the American Heart Association, about 80% of heart disease is preventable. That’s the focus of preventive cardiology.
Preventive cardiology is a subspecialty of medicine that focuses on lowering the risk of heart disease before a diagnosis or incident, or — for patients who already have had a heart attack or stroke — reducing the chance of the disease worsening or having another event.
Dr. Hornick says preventive cardiology is especially important for anyone with a family member who experienced early coronary disease. This includes:
A father or male relative who had a heart attack or needed a stent before age 55.
A mother or female relative who had a heart attack or needed a stent before age 65.
“With early identification, we can take steps to control risk factors and prevent heart disease from developing,” says Dr. Hornick.
EVALUATING RISK
UPMC Passavant offers a wide range of services to help patients determine their risk of cardiovascular disease and improve their heart health.
Preventive cardiology begins with a comprehensive heart disease risk assessment. This includes an evaluation of the following:
Existing medical conditions (such as diabetes or prediabetes)
Family history of heart disease
Lifestyle choices: diet, exercise
Traditional risk factors:
— Blood pressure
— Cholesterol/lipid profile
— Glucose levels
— Obesity
— Smoking history
Specific lab tests are also used to look for forms of high cholesterol that don’t show up on normal lipid panels. Another useful test is the coronary artery calcium scan to detect calcium deposits — an early sign of heart disease.
INDIVIDUALIZED TREATMENT
“Once we identify the risk, we work with the patient to design a preventive program based on individual needs,” says Dr. Hornick. “We are able to impact patients and prevent future cardiac events.”
Treatment plans typically involve lifestyle changes, such as weight loss, exercise, and reducing saturated fats. UPMC Passavant’s preventive cardiology team works collaboratively with other specialists, including endocrinologists, vascular experts, exercise physiologists, and weight loss specialists.
Dr. Hornick, who underwent special training in the treatment of advanced lipidology, works closely with patients who have trouble controlling their cholesterol with statins and other medicine. He also helps those who are unable to tolerate statin side effects to find alternative medications that lower cholesterol.
Treatment options include:
Blood pressure management
Cholesterol and triglyceride management
Diabetes management
Exercise counseling
Genetic counseling
Nutrition counseling
Smoking cessation counseling
Stress testing
Find a cardiologist, surgeon, or provider close to where you live or work at UPMC.com/NorthHVI.




















Comments